Disqualifying Factors for Dental Implant Eligibility
.png)
.png)
The most common disqualifying factors for dental implant eligibility are insufficient jawbone density, active gum disease, uncontrolled diabetes, heavy smoking, and certain medications that interfere with bone healing. Most of these are not permanent barriers. Many patients who are told they do not qualify today can become strong candidates after addressing the underlying issue. This article covers every major factor that affects implant eligibility, what the research says about each one, and how a thorough evaluation helps determine the clearest path forward.
What Disqualifies You from Getting Dental Implants?
The factors that disqualify you from getting dental implants fall into three main categories: oral health conditions, systemic medical conditions, and lifestyle factors. The most absolute disqualifiers involve active infections or diseases that would make surgery unsafe right now. The relative disqualifiers are conditions that raise the risk of failure but can often be managed or treated before implant placement begins.
Dental implants have a success rate of 95 to 98% at the 10-year mark according to a large-scale cohort study published in the Journal of Periodontology tracking over 10,800 implants in more than 4,200 patients. That number reflects patients who were properly screened and qualified before surgery. The patients who fall outside that success window are almost always those who were not ideal candidates to begin with. This is exactly why eligibility screening is not a hurdle. It is what makes good outcomes possible.
We take every new patient through a complete evaluation before recommending dental implants, including a review of their medical history, a full oral health assessment, and bone imaging. The goal is always to find a path forward, not to turn people away.
What Makes You Not a Candidate for Implants?
The conditions that make you not a candidate for implants can be divided into those that are temporary and those that are permanent. Temporary disqualifiers include active gum disease, uncontrolled blood sugar, active infection, and insufficient bone that can be corrected with a graft. Permanent or difficult-to-resolve disqualifiers include severe jawbone loss with no grafting potential, recent head and neck radiation therapy, and certain blood clotting disorders that make surgery unsafe regardless of preparation.
The important distinction is that most patients who are initially told they do not qualify fall into the temporary category. They need a preparatory step first, not a permanent no.
How Does Insufficient Jawbone Density Affect Dental Implant Eligibility?
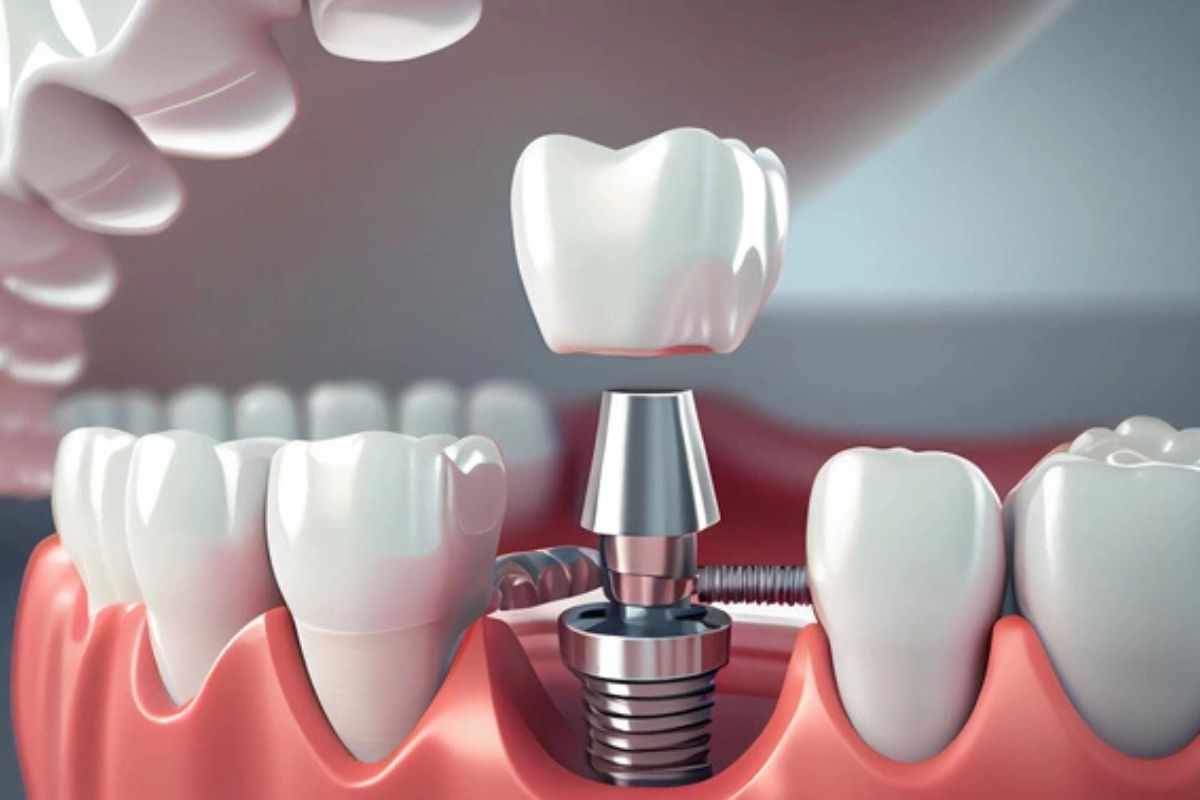
Insufficient jawbone density affects dental implant eligibility because the titanium post needs a strong, dense bone to fuse with during the osseointegration process. If the bone is too thin, too soft, or has too little volume, the implant cannot achieve the initial stability it needs to integrate properly. Research published in the Journal of Family Medicine and Primary Care found that implants placed in Type IV bone, the softest and least dense bone category, had a failure rate of 20.6%. Implants placed in denser Type II and Type III bone showed survival rates of 98.9% and 98.2% respectively.
Bone loss after tooth loss happens faster than most people expect. When a tooth root is no longer present to stimulate the jawbone, the bone in that area begins to shrink through a process called resorption. The longer a tooth has been missing without replacement, the more bone has typically been lost. This is one of the strongest reasons to address a missing tooth sooner rather than later. Our existing post on how long dental implants last explains in detail how bone quality shapes long-term implant success.
The good news is that insufficient bone is often solvable. Bone grafting procedures can restore volume and density to areas that have resorbed, creating a foundation strong enough to support an implant. A sinus lift is a specialized form of grafting used when the upper jaw does not have enough height near the back teeth. These preparatory procedures add time to the overall treatment plan but open the door for patients who would otherwise not qualify.
.png)
Why Do Dental Implants Get Rejected?
Dental implants get rejected when the body fails to properly integrate the titanium post into the jawbone, a problem called failed osseointegration. This happens most often in the first few months after surgery. The leading causes include poor bone quality, active infection at the implant site, smoking, uncontrolled diabetes, and certain medications that interfere with bone metabolism.
According to research published in PMC, a meta-analysis on smoking found that smokers have a relative risk of implant failure 1.92 times higher than non-smokers. Head and neck radiation therapy was associated with an even higher relative risk of 2.28. These are not small differences. They are the reason we ask about every medication, every health condition, and every lifestyle habit before planning surgery. A dental implant that is rejected must be removed, and the site must heal before a second attempt can be made, which is why thorough screening matters so much upfront.
How Does Gum Disease Affect Dental Implant Candidacy?
Active gum disease directly affects dental implant candidacy because it creates an infected environment around the very tissue the implant must fuse with. Periodontal disease destroys the bone and gum tissue that support teeth. Placing an implant into a mouth with active periodontal disease is placing it into an environment already working against it. The bacteria responsible for gum disease are the same bacteria that cause peri-implantitis, a serious infection around the implant that is the leading cause of late implant failure.
Gum disease does not automatically disqualify you permanently. It disqualifies you from getting an implant right now. Treatment for periodontal disease, including deep cleaning procedures and, in more advanced cases, surgical intervention, can bring the infection under control. Once the gum tissue is healthy and stable, implant placement becomes a much safer proposition. A professional cleaning is often the starting point in preparing a patient with mild gum disease for implant candidacy. If you are exploring all your tooth replacement options while preparing for implants, the comparison between a dental bridge vs. implant can help clarify which direction fits your situation best.
How Many People Reject Dental Implants?
The overall failure rate for dental implants is between 2% and 10% depending on the study and patient population. One large study analyzing over 9,000 implants found a survival rate of 96.13%, placing the failure rate at approximately 3.87% over five years. A 2026 study published in the Journal of Functional Biomaterials found a failure rate of just 2.17% for implants placed with bone grafting, showing that even patients who needed preparatory work achieved excellent outcomes. These numbers confirm that outright rejection is uncommon in properly screened candidates.
Upper jaw implants fail at higher rates than lower jaw implants. Research cited in Bite Club Chicago found that 83% of failed implants occurred in the upper jaw, where bone is naturally less dense, especially near the sinuses. This is why implant planning varies by location in the mouth, not just by overall health status.
.png)
Does Diabetes Disqualify You from Dental Implants?
Uncontrolled diabetes disqualifies you from dental implants, but well-controlled diabetes does not. This is a critical distinction that many patients do not hear clearly. The problem with diabetes and implants is specifically about blood sugar levels and their effect on healing. High blood glucose impairs immune function, slows tissue repair, and increases the risk of infection after surgery. All three of these effects work directly against osseointegration.
When diabetes is well managed, the picture changes significantly. A systematic review found 96 to 97% one-year implant survival rates in patients with well-managed Type 2 diabetes, comparable to non-diabetic patients. Research published in PMC confirms that the direct impact of diabetes on implant failure is closely tied to how well blood sugar is controlled, not the diagnosis itself. Patients with an HbA1c below 7% are generally considered appropriate candidates after medical clearance from their physician.
If your diabetes is currently not well controlled, your dentist and your primary care physician can work together to stabilize your blood sugar before and after surgery, bringing your risk profile much closer to that of a non-diabetic patient.
At What Age Are Dental Implants Not Recommended?
Dental implants are not recommended for patients whose jawbones are still growing and developing, which typically means anyone under the age of 17 to 18 for girls and 18 to 21 for boys. The jawbone must be fully mature before an implant post is placed, because a post placed in a still-developing jaw will not move with the bone as it grows. This can lead to the implant sitting in the wrong position as the surrounding bone matures.
There is no upper age limit for dental implants. Older patients can and do receive implants successfully. However, research shows that seniors between the ages of 66 and 80 have higher early failure rates of approximately 14.6% compared to under 5% for younger adults, largely due to lower bone density and slower healing. This does not mean older patients should not pursue implants. It means the pre-surgical evaluation needs to be especially thorough, with close attention to bone quality and any systemic health factors that could affect healing.
Disqualifying FactorTemporary or Permanent?Path to EligibilityInsufficient jawbone (volume or density)Usually temporaryBone grafting or sinus lift before implant placementActive gum diseaseTemporaryPeriodontal treatment to resolve infection firstUncontrolled diabetesTemporaryStabilize blood sugar; medical clearance requiredHeavy smokingTemporaryQuit or significantly reduce before and after surgeryBisphosphonate medicationsRelative risk; case-by-caseFull medication review; possible drug holiday with physicianHead and neck radiation (recent)Difficult; relative contraindicationTiming and dose reviewed with oncology teamJawbone still developing (young patients)TemporaryWait until full skeletal maturitySevere uncontrolled autoimmune diseaseRelative; depends on stabilityMedical management and specialist clearance required
Sources: Journal of Periodontology (22-year cohort study); PMC meta-analysis on smoking and radiotherapy risk (Moraschini et al.); Journal of Family Medicine and Primary Care bone density failure data; PMC systematic review on bisphosphonates and implant failure.
Does Smoking Disqualify You from Dental Implants?
Heavy smoking significantly increases implant failure risk but does not automatically disqualify you permanently. Smoking reduces blood flow to the gums and bone, slows the healing process, and increases the risk of peri-implantitis. A meta-analysis published in PMC found that smokers have a relative risk of implant failure nearly twice that of non-smokers (RR 1.92). This is one of the most consistent findings across implant research.
Patients who quit smoking before implant surgery and remain smoke-free during the healing period see substantially better outcomes. Research from Omega Dental Houston cites that quitting at least two weeks before surgery and remaining smoke-free for eight weeks after gives the healing process the best chance to proceed without complications. Patients who are willing to make this commitment can still be good candidates for implants with close monitoring throughout treatment.
What Is the Most Painful Part of Getting a Dental Implant?
The most painful part of getting a dental implant is the recovery period in the first 3 to 5 days after the titanium post is placed, not the surgery itself. During the procedure, local anesthesia keeps the area fully numb, and patients feel pressure but not pain. After the anesthesia wears off, soreness and swelling around the implant site are common and typically peak in the first 2 to 3 days. Most patients manage this comfortably with over-the-counter pain medication.
Patients who require bone grafting before implant placement may experience a slightly longer recovery because the graft site also needs time to heal. In most cases, the discomfort is manageable and temporary. The long-term result, a stable, permanent tooth that looks and functions naturally, is what makes the short recovery period worthwhile for the vast majority of patients.
.png)
How Do Medications Affect Dental Implant Eligibility?
Certain medications affect dental implant eligibility by interfering with bone healing, blood clotting, or immune function. The most important category to disclose before implant planning is bisphosphonates, a class of drugs prescribed for osteoporosis and other bone conditions. These medications slow bone remodeling, which is the same biological process that allows the jawbone to fuse around a titanium post. A systematic review and meta-analysis published in MDPI Materials analyzing 33 studies found that patients taking bisphosphonates had a higher implant failure risk compared to patients not on these medications (OR 1.653).
Bisphosphonate use is not an absolute disqualifier, but it requires careful evaluation. The type of bisphosphonate, how long the patient has been taking it, the dose, and whether it is taken orally or intravenously all influence the risk level. Intravenous bisphosphonates (used in cancer treatment) carry significantly higher risk than oral bisphosphonates (used for osteoporosis). In some cases, a physician-supervised drug holiday before surgery reduces the risk enough to proceed safely.
Other medications that require disclosure include blood thinners, corticosteroids, immunosuppressants, and certain antidepressants. We review every medication at your initial consultation because a complete picture of your health is what allows us to plan safely. A thorough dental exam always includes a full medication review before any treatment planning begins.
Does Getting the Screw for an Implant Hurt?
Getting the screw, which is the titanium post placed into the jawbone, does not hurt during the procedure because the area is fully numbed with local anesthesia. You will feel pressure and hear sounds from the drilling and placement, but not pain. Most patients report that the experience is far more comfortable than they expected. The soreness that follows in the days after surgery is normal and manageable. It is the body's healing response, not a sign that anything went wrong.
Can You Fix a Disqualifying Factor and Then Get Implants?
Yes, you can fix most disqualifying factors and then get implants. This is the most important thing to understand about implant eligibility. The majority of factors that prevent someone from getting an implant today are addressable with the right preparation. Bone grafting restores lost bone volume. Periodontal treatment clears active gum infection. Blood sugar management brings diabetic patients into a safe range. Quitting smoking removes one of the biggest controllable risk factors.
The timeline for becoming eligible varies. Bone grafting and healing can take 4 to 6 months before an implant can be placed into the grafted site. Gum disease treatment may take weeks to months depending on severity. These preparatory steps add time, but they are what turn a "not yet" into a successful implant outcome. Patients who take the time to get the foundation right before implant placement consistently achieve better long-term results. Once the implant post is fully integrated, a custom dental crown is placed on top, completing the restoration with a natural-looking finish.
If you have been told you do not qualify for implants, the first question worth asking is why. If the answer is bone loss, gum disease, or blood sugar, those are manageable. We have helped many patients in Hialeah work through exactly these preparatory steps and end up with stable, long-lasting implants. If bridges or dentures are needed in the meantime, a dental bridge can restore function while a longer-term plan is developed.
How Long Does It Take to Get Used to Full Mouth Dental Implants?
Most patients get used to full mouth dental implants within 3 to 6 months after the final restorations are placed. The adjustment period involves the mouth adapting to the feel of the new teeth during chewing and speaking, and the surrounding tissues settling around the implant posts. Bite pressure can feel different at first because the sensory feedback from implants is slightly different than from natural teeth. This normalizes as the brain adjusts to the new stimulation pattern.
Full mouth implant cases involve a longer overall timeline than single implants because multiple posts must osseointegrate, which takes 3 to 6 months per site. Many full mouth patients receive temporary teeth during this healing phase so they are never without function. By the time the final crowns or prosthetics are placed, the posts are fully integrated and the mouth is ready to function normally. Most patients find that by 6 months post-restoration, the implants feel completely natural.
.png)
Frequently Asked Questions
What Is the 3/2 Rule for Dental Implants?
The 3/2 rule for dental implants is a clinical guideline referring to the minimum bone dimensions needed to safely place an implant: at least 3mm of bone width surrounding the implant and at least 2mm of bone clearance from vital structures like nerves and the sinus floor. This guideline helps surgeons avoid damaging adjacent structures and ensures the implant has adequate bone support on all sides. If imaging shows that bone dimensions fall short of these minimums, grafting or alternative planning is required before placement can proceed safely.
What Is the Rule of 3 in Implant Dentistry?
The rule of 3 in implant dentistry refers to the recommended minimum of 3mm of bone between an implant and any adjacent tooth, nerve, or anatomical structure. This spacing is considered the safe threshold that protects neighboring structures from being compromised by the implant post. Violating this spacing during placement can lead to nerve involvement, damage to adjacent tooth roots, or implant failure due to insufficient bone support. Cone beam CT scans allow dentists to measure these dimensions precisely before committing to a placement plan.
How Many 70-Year-Olds Still Have All Their Teeth?
Very few 70-year-olds still have all of their natural teeth. According to national dental research data, approximately 69% of American adults between the ages of 35 and 44 have already lost at least one permanent tooth, and by age 74, roughly one in four American adults has lost all of their teeth. Complete tooth retention into the 70s is uncommon and is associated with lifelong excellent oral hygiene, no history of gum disease, and regular preventive dental care. This data highlights why tooth replacement options like implants are so relevant to older adults.
What Destroys Teeth the Most?
The conditions that destroy teeth the most are untreated gum disease, tooth decay, and bruxism (teeth grinding). Periodontal disease is the leading cause of tooth loss in adults because it progressively destroys the bone and gum tissue that hold teeth in place. Decay left untreated spreads to the inner pulp and eventually makes a tooth non-restorable. Bruxism places extreme mechanical stress on teeth over time, causing fractures, worn enamel, and cracked roots. All three of these are also factors that affect implant eligibility, since they reflect the overall health of the oral environment an implant would be placed into. Keeping up with preventive dentistry is the most effective way to protect both natural teeth and implants long-term.
Can You Get Implants If You Have Had Teeth Extracted Recently?
Yes, you can get implants after a recent tooth extraction, and in some cases an implant can be placed immediately at the time of extraction if bone conditions allow. Immediate implant placement is not appropriate for every extraction site, particularly when infection was present or when bone volume is insufficient at the time of removal. When immediate placement is not suitable, a healing period of 2 to 4 months is typically recommended before implant surgery, which gives the extraction socket time to fill in with new bone. Your dentist will use imaging to assess whether the site is ready and whether any grafting is needed to support the implant. You can learn more about what to expect from the removal process itself on our tooth extractions page.
Wrapping It Up
Most factors that disqualify someone from dental implants are not permanent. Insufficient bone, active gum disease, uncontrolled blood sugar, and smoking are the most common barriers, and every one of them has a path to resolution with the right preparation and care. The key is a thorough evaluation upfront so the right plan is in place before any surgery begins.
Implant success rates above 95% at 10 years are not accidental. They are the result of careful patient selection and proper preparation. The patients who struggle with implants are almost always those who skipped the screening or whose underlying conditions were not addressed first. For patients who need to replace several teeth while preparing for implants, full or partial dentures can serve as a functional interim solution.
At Castellanos Dental, we walk every patient through a full eligibility evaluation before recommending any implant treatment. If you have questions about whether you qualify or what steps might be needed to get there, we are glad to help you find out.
.png)
.png)
.png)
.png)
.svg)
.png)

.png)
.png)

.png)
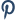





.png)
.png)
.png)
.png)

.png)
.png)
.svg)



